Anal warts
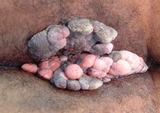 Anal warts are caused by the human papillomavirus (HPV), which has been linked to increased risk of cervical and anal cancers. Infection occurs when secretions collect in the anal area, causing multiple warts of various sizes. Although individuals who engage in anal intercourse have a higher frequency of perianal warts, the majority of patients with perianal warts have not engaged in anal intercourse.
Anal warts are caused by the human papillomavirus (HPV), which has been linked to increased risk of cervical and anal cancers. Infection occurs when secretions collect in the anal area, causing multiple warts of various sizes. Although individuals who engage in anal intercourse have a higher frequency of perianal warts, the majority of patients with perianal warts have not engaged in anal intercourse.
Anal warts can be treated with agents such as topical Fluorouracil (Efudex) and Imiquimod (Aldara), but they have a low cure rate. Trichloroacetic acid (TCA) and cryotherapy with liquid nitrogen are more successful but may require several treatments, especially with large lesions. Radiofrequency and laser therapy produce 90 percent cure rates and is the preferred treatment method by Dr.Shu.
Fissures
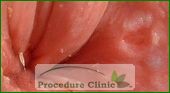 A fissure is a small cut or split in the anoderm often caused by a painful, hard bowel movement. Pain from the bowel movements usually lasts for about an hour before either subsiding or continuing at a lesser degree. Fissures are typically located anterior or posterior to the anus. When fissures are found laterally, other uncommon causes should be considered.
A fissure is a small cut or split in the anoderm often caused by a painful, hard bowel movement. Pain from the bowel movements usually lasts for about an hour before either subsiding or continuing at a lesser degree. Fissures are typically located anterior or posterior to the anus. When fissures are found laterally, other uncommon causes should be considered.
Treatment for an acute fissure is quite simple when it is identified within a month of onset. 85% to 90% patients respond well to anal care measures. Once a fissure has become chronic,, it is more difficult to treat. Topical solutions such as nifedipine gel or nitroglycerin ointment have about 50 percent success rates. Most patients couldn’t tolerate the headache side effect from nitroglycerin ointment. Chronic fissures are usually treated with lateral sphincterectomy, a surgical office procedure that cures 90-95% of cases. A chemical sphincterectomy using a botox injection into the anal sphincter is an alternative option.
Anal fistula
Anal fistulas are usually caused by an abscess in the anal area due to infection. Patients often experience recurrent infection with intermittent drainage of pus from the anal’s opening. Abscess formation can be easily treated using incision and drainage (I&D), antibiotics, and frequent Sitz baths.
Patients with chronic complicated fistulas are treated with a fistulotomy or fistulectomy, including cutting setons, advancement flaps or muscle repair and fibrin glue injection.
Anal abscesses
Abscesses also begin as an infection in the anal glands. The patients usually have severe rectal pain with local redness and swelling. Superficial perianal abscesses are easily drained in the office under local anesthesia, it resolve after treated with antibiotics and anal care measures.
The infection may track through the sphincter muscles to enter the surrounding space or above levator muscle. The patients usually have toxic signs and fever. and these abscesses are difficult to diagnose and require a high index of suspicion.
Hemorrhoids
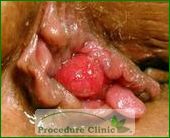 Everyone has had a normal hemorrhoidal tissue in their rectum and anus. It’s only when your hemorrhoidal veins enlarge and become varicose veins that they’re considered abnormal or diseased. There are three types of hemorrhoids – internal, external, and mixed. Internal hemorrhoids form above the dentate line, while external hemorrhoids form below the dentate line. Mixed hemorrhoids can either refer to lesions formed at the dentate line, or to the presence of both internal and external hemorrhoids.
Everyone has had a normal hemorrhoidal tissue in their rectum and anus. It’s only when your hemorrhoidal veins enlarge and become varicose veins that they’re considered abnormal or diseased. There are three types of hemorrhoids – internal, external, and mixed. Internal hemorrhoids form above the dentate line, while external hemorrhoids form below the dentate line. Mixed hemorrhoids can either refer to lesions formed at the dentate line, or to the presence of both internal and external hemorrhoids.
External hemorrhoids are those occur outside the anal verge. External hemorrhoids usually affect the cleansing after the bowel movement and cause the skin irritation and itching. The thrombosed external hemorrhoids are sometimes very painful if the varicose veins rupture and the blood clots develop, it is often accompanied by swelling and irritation. These hemorrhoids are typically treated with either incision and removal of the clot or with external hemorrhoidectomy. Simply draining the clot can lead to recurrence, so it is generally recommended to completely excise the thrombosed hemorrhoids.
Internal hemorrhoids are graded from I to IV based on the degree of prolapse. Grade I hemorrhoids have no prolapse. Grade II lesions bulge with defecation but then recede spontaneously. Grade III hemorrhoids require digital replacement after prolapsing, while grade IV hemorrhoids cannot be replaced once prolapsed.
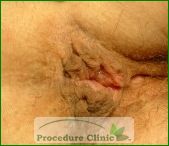
Anal Tags
Anal tags usually arise from previous external hemorrhoids and may periodically cause itching, anxiety or hygienic problems. The tags can be surgically removed using local anesthesia.
Anal Polyps
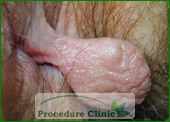 Anal polyps are the growth in the anal canal that must be removed for the biopsy. Further examination with colonoscopy is required for polyps confirmed to be adenomatous in order to check for proximal lesions in the rectum and colon. Hypertrophied Papillae is anal papilla at the dentate line, often confused with a polyp. Treatment is generally not indicated for confirmed hypertrophied papillae.
Anal polyps are the growth in the anal canal that must be removed for the biopsy. Further examination with colonoscopy is required for polyps confirmed to be adenomatous in order to check for proximal lesions in the rectum and colon. Hypertrophied Papillae is anal papilla at the dentate line, often confused with a polyp. Treatment is generally not indicated for confirmed hypertrophied papillae.
Cancer of the Anus and Rectum
Anal cancer is account for 2% of cancer in the gastrointestinal tract. Anal or rectal cancer generally do not produce any pain; an external or internal mass may be palpable. Some lesions are so soft that they are missed on palpation. Anal cancers are staged and treated differently from rectal cancers. Anal cancer can take several forms including ulcers, polyps or verrucous growths; treatment is typically a combination of surgery, chemotherapy and pelvic radiation.




