Hemorrhoids Online Registration
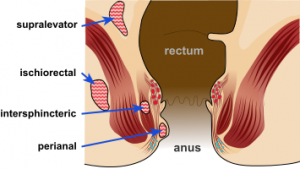 Anorectal abscesses occur when anal glands in the lining of the anal canal near the opening of the anus become infected. When bacteria from the gut passes the anal sphincter barrier (which usually keeps such bacteria away from the rectum) via an anal crypt and into the surrounding rectal tissue, an abscess of varying severity and depth forms.
Anorectal abscesses occur when anal glands in the lining of the anal canal near the opening of the anus become infected. When bacteria from the gut passes the anal sphincter barrier (which usually keeps such bacteria away from the rectum) via an anal crypt and into the surrounding rectal tissue, an abscess of varying severity and depth forms.
Anal abscesses most commonly occur in men, as well as patients who are in their 30s and 40s. Most abscesses can be identified through an initial physical exam and digital rectal examination, although deep abscesses may require a CT scan, MRI scan, or ultrasonography to confirm. A digital rectal examination involves the doctor inserting a finger into the rectum to feel out the presence of an abscess.
What’s the Difference Between Anal Abscesses and Hemorrhoids?
Although both hemorrhoids and anal abscesses appear to be tissue lumps protruding from the rectum, they are two very different conditions. Anal abscesses are an infection around the opening of the anus or deep in the rectum, where there is pus. They are commonly mistaken for hemorrhoids but are more painful and can lead to fever. An anal abscess is an acute disease rather than a chronic condition, and it’s important to seek medical attention if symptoms are found.
Treatment
Surgical incision and drainage should be performed ASAP, as antibiotics are ineffective at this stage of the infection. Delaying surgery can result in tissue destruction, fibrosis (scar tissue formation), and impaired anal continence.
Drainage involves making a small incision above the abscess as close to the anus as possible. The gauze is removed after 24 hours, and the patient then focuses on postoperative care—warm sitz baths three times daily and after bowel movements, stool softeners, and pain medication as needed.



