Hemorrhoids Online Registration
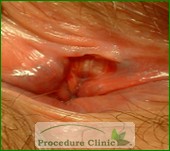 Although hemorrhoids and anal fissures are both related to rectal pain and rectal bleeding, they are two very different conditions. Hemorrhoids are usually only mildly painful and aren’t always related to bowel movements. Anal fissures, however, produce sharp rectal pain during bowel movements.
Although hemorrhoids and anal fissures are both related to rectal pain and rectal bleeding, they are two very different conditions. Hemorrhoids are usually only mildly painful and aren’t always related to bowel movements. Anal fissures, however, produce sharp rectal pain during bowel movements.
What’s an Anal Fissure?
An anal fissure is a tear in the anal canal in the lower rectum. They’re usually caused by trauma from a hard or painful bowel movement and lack of dietary fiber. Symptoms include severe rectal pain during bowel movements, which worsens with constipation. Slight rectal bleeding may also occur.
Diagnosis requires a physical exam using an anoscopy, as fissures cannot be directly observed. However, because the use of an anoscopy can be quite painful for anal fissure patients, your doctor may simply treat the fissure based on symptoms alone. However, patients may need a colonoscopy to ensure that no underlying conditions are causing the rectal bleeding.
Treatments
Non-Surgical Treatments
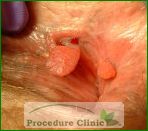
Initial treatment is generally based on lifestyle changes, with the goal of relieving constipation and fixing hard bowel movements. Patients should take stool-bulking agents like fiber supplements and stool softeners, as well as laxatives to encourage regular bowel movements. Sitz baths after bowel movements are also effective in healing symptoms. Patients should also drink more fluids, exercise regularly and avoid straining during bowel movements.
If these first-line treatments do not work, the patient may be directed to use 0.4% nitroglycerine (NTG) ointment or compounding medication Nifedipine gel in conjunction with the previously listed treatments to reduce discomfort.
 If the fissure fails to heal on its own within six to eight weeks, a Botox injection is most likely the next step. Due to its muscle-relaxation effects, Botox is often used on the internal anal sphincter for roughly three months to allow the anal fissure to heal. This method has a 90 percent success rate but is NOT covered by your insurance provider.
If the fissure fails to heal on its own within six to eight weeks, a Botox injection is most likely the next step. Due to its muscle-relaxation effects, Botox is often used on the internal anal sphincter for roughly three months to allow the anal fissure to heal. This method has a 90 percent success rate but is NOT covered by your insurance provider.
Surgery
If Botox treatments prove ineffective, then a partial anal sphincterotomy may be needed. This procedures involves cutting a segment of the anal sphincter muscle to reduce spasms and promote healing, and may also include removing the fissure and any scar tissue resulting from it. Although very rare, cutting the anal sphincter may lead to losing one’s ability to control bowel movements.



