Hemorrhoids Online Registration
- What is a Hemorrhoid?
- What is Infrared Coagulation Treatment (IRC)?
- How Do You Temporarily Alleviate Hemorrhoid Symptoms Before Seeing a Doctor?
- How Common Are Hemorrhoids?
- What Are the Main Symptoms of Hemorrhoids?
- How Do You Manage Hemorrhoids During Pregnancy?
- What Are the Best Treatments for Hemorrhoids?
- What is Rubber Band Ligation?
- Does Pregnancy Cause Hemorrhoids?
- When Should I Call a Doctor From the Hemorrhoid Clinic?
- What Are Common Causes of Rectal Lumps?
- What is the Easy Hemorrhoid Care™ (EHC) Program?
- What Are Common Causes of Anal Itching?
- What Should I Know About Anal Cancer?
- How Do You Differentiate Anal Fissures From Hemorrhoids?
- Why Are Infected Hemorrhoids So Rare?
- What is the Correct Way to Use Hemorrhoid Cream?
- What’s the Difference Between Hemorrhoids and Anal Abscesses?
- What Are Common Causes of Minor Rectal Bleeding?
- How Do You Treat External Thrombosed Hemorrhoids?
- What is Proctalgia Fugax (Fleeting Rectal Pain)?
- What is the Recovery Process for an External Hemorrhoidectomy?
- How Do You Find a Qualified Hemorrhoid Doctor?
- What Are the Best & Worst Foods to Eat When You Have Hemorrhoids?
- What Are Everyday Habits That Contribute to Hemorrhoid Development?
- What Kind of Exercises Help Alleviate Hemorrhoid Symptoms?
What is a Hemorrhoid?
Believe it or not, everyone has had a normal hemorrhoidal tissue in their rectum and anus. Hemorrhoids are actually part of our normal anatomy. They are clusters of vascular tissue, smooth muscle, and connective tissue lined by the normal epithelium of the anal canal.
 We used to believe that hemorrhoidal bleeding is venous. Now the evidence indicates that hemorrhoidal bleeding is arterial, which is supported by the bright red color and arterial pH of the blood.
We used to believe that hemorrhoidal bleeding is venous. Now the evidence indicates that hemorrhoidal bleeding is arterial, which is supported by the bright red color and arterial pH of the blood.
There are two different types of hemorrhoids: internal and external hemorrhoids based on their anatomic origin and their position relative to the dentate line.
| Internal Hemorrhoids | External Hemorrhoids | |
| Surface Epithelium | Columnar epithelium | Squamous epithelium |
| Nerve Supply | Not cutaneous nerves | Somatic sensory nerves |
| Position relative to the dentate line | Above the dentate line | Below the dentate line |
Internal hemorrhoids are not supplied by cutaneous nerves and therefore cannot cause sharp pain. hemorrhoids can be found at any position within the rectum, and many have 3 main cushions around the anal canal.
Under normal circumstances, hemorrhoids vascular tissue helps to assist in defecation during the bowel movement by providing important sensory information, enabling the differentiation between solid, liquid, and gas, and keeping some continence or control of our gas.
It’s only when your hemorrhoids enlarge and prolapsed that they’re considered abnormal or diseased.
What is Infrared Coagulation Treatment (IRC)?
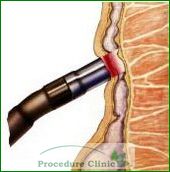 The most common treatment method for hemorrhoids is infrared coagulation (IRC), a minimally-invasive, non-surgical procedure. A small probe is inserted into the anus to flash infrared light onto the surface of the hemorrhoid. The heat from this infrared probe burns the hemorrhoid and creates scar tissue that cuts off its blood supply, causing it to shrink and die.
The most common treatment method for hemorrhoids is infrared coagulation (IRC), a minimally-invasive, non-surgical procedure. A small probe is inserted into the anus to flash infrared light onto the surface of the hemorrhoid. The heat from this infrared probe burns the hemorrhoid and creates scar tissue that cuts off its blood supply, causing it to shrink and die.
IRC offers major advantages over other hemorrhoid treatment methods:
While patients may feel some heat and pain during the procedure, discomfort is usually brief and minimal. Following IRC, there may be a temporary urge to defacate or a feeling of fullness in the lower abdomen. Rectal bleeding may also occur, but this should stop on its own.
How Do You Temporarily Alleviate Hemorrhoid Symptoms Before Seeing a Doctor?
As you wait for your doctor’s appointment, you can temporarily treat hemorrhoid symptoms with the following steps:
How Common Are Hemorrhoids?
Due to lack of studies and documentation on hemorrhoids, the exact percentage is unknown. However, it’s estimated that roughly half of Americans develop hemorrhoids by age 50, and about 10 million people in the US are affected, with 1 million new cases each year.
While hemorrhoids can develop at any age, most cases occur in patients over 30, with a peak in those between 45-60 years old. External hemorrhoids tend to be more common in younger adults. Although men seem to be more likely to seek medical attention, pregnancy can increase the chance of symptomatic hemorrhoids, as well as thrombosis, in women.
There are no indicative factors to identify which individuals are more predisposed to hemorrhoids. Caucasians are affected by, and seek treatment for, hemorrhoidal disease more often than other races. Those who 1) live in rural areas and 2) have higher socioeconomic status seem to be more prone to developing hemorrhoids.
What Are the Main Symptoms of Hemorrhoids?
While hemorrhoidal symptoms are common and typically not a serious concern, all patients should be examined for signs of possible cancer and other associated diseases. The four primary symptoms of hemorrhoids include rectal pain, bleeding, anal itching, and a rectal mass/lump.
Anal Itching – The most common complaint from patients, anal itching often comes and goes but can worsen due to scratching or excessive cleaning of the anal area. When chronic itching occurs, the perianal area becomes white with fine fissures. Treatment includes taking antihistamine as a sedative before sleeping to prevent unconscious scratching, or applying a topical corticosteroid to alleviate the itching.
Anal pain – Aching, irritating, and spasmodic pain are common complaints. Immediate onsets of intense pain accompanied by a palpable mass are usually signs of an external thrombosed hemorrhoid, while internal hemorrhoids aren’t usually painful. Patients who also suffer from an anal fissure may feel sharp pain and rectal bleeding during intense, forced bowel movements.
Rectal Lump – While a lump can be caused by anything from anal warts and fissures to cancer, hemorrhoids are probably the most common reason for a rectal lump. For an internal hemorrhoid, the lump usually gets bigger and more prolapsed right after a bowel movement. For thrombosed external hemorrhoids, painful and blue-colored lumps appear due to the ruptured hemorrhoidal veins and blood clots.
Rectal Bleeding – Common causes of bleeding are internal hemorrhoids, ruptured thrombosed external hemorrhoids, fissures, diverticulosis, colon cancer, colitis, polyps and angiodysplasias. Older patients and those with significant family history of bowel disease/cancer should consider further examination, as well as patients previously treated for rectal bleeding but continue to experience bleeding.
How Do You Manage Hemorrhoids During Pregnancy?
 Hemorrhoids afflict 20 to 50 percent of all pregnant women in Minnesota. They can strike during first-time pregnancies and also recur following childbirth. Hemorrhoids usually worsen in the third trimester, immediately after labor, or in conjunction with constipation. Pressure on the pelvic veins, constipation, and increased progesterone increase the chance of hemorrhoids during pregnancy. Below are home remedies that can help alleviate symptoms:
Hemorrhoids afflict 20 to 50 percent of all pregnant women in Minnesota. They can strike during first-time pregnancies and also recur following childbirth. Hemorrhoids usually worsen in the third trimester, immediately after labor, or in conjunction with constipation. Pressure on the pelvic veins, constipation, and increased progesterone increase the chance of hemorrhoids during pregnancy. Below are home remedies that can help alleviate symptoms:
If these suggestions don’t help, or your hemorrhoids get worse, consult with hemorrhoid care expert Dr. Shu in Minneapolis, MN. He provides one stop hemorrhoid care with multiple treatment modalities.
What Are the Best Treatments for Hemorrhoids?
Hemorrhoid diseases include internal hemorrhoids (graded from 1 to 4 based on the degree of prolapse), external hemorrhoids, anal tags, thrombosis of hemorrhoids and mixed hemorrhoids (internal and external). Because no single treatment modality can fix all hemorrhoids, a hemorrhoid clinic will offer multiple treatment modalities to meet a patient’s specific needs and provide complete care. If you are treated with a single modality, without regard for severity, type, and associated anorectal conditions, it leads to poor and incomplete results.
Internal Hemorrhoids, Grade 1
Very early-stage hemorrhoids can usually be treated via dietary and lifestyle changes, which form the base for all hemorrhoid treatment types:
Internal Hemorrhoids, Grade 1-2
Infrared coagulation (IRC) is a non-surgical treatment that is fast, well tolerated, and remarkably complication-free. The infrared light quickly coagulates the hemorrhoid’s blood supply, causing it to shrink and recede.
Internal Hemorrhoids, Grade 3
These can be treated with a combination of infrared coagulation and rubber band ligation (banding). Rubber band ligation is widely used for treating more advanced (more prolapsed) internal hemorrhoids where rubber bands are placed around the prolapsed hemorrhoidal tissue. Over time, the tissue dies off. Rubber band ligation downgrades the hemorrhoid to grade 1 or 2, so follow-up IRC treatments may be needed afterward.
Internal Hemorrhoids, Grade 4
A hemorrhoidectomy surgically removes the tissue that causes bleeding or protrusion. It is done in a doctor’s office, surgical center or hospital under anesthesia and may require a period of inactivity.
External Hemorrhoidal Tags (Anal Tags)
Small and asymptomatic tags don’t require any treatment. If symptomatic, anal tags can easily be removed in the office using a local anesthetic and a radiofrequency device.
Thrombosed External Hemorrhoids
These are typically treated with either incision to remove the clot or with an external hemorrhoidectomy. Simply draining the clot temporarily relieves the pain but can also lead to hemorrhoid recurrence, so it’s ideal for patients with multiple thromboses to completely excise the thrombosed hemorrhoids.
External Hemorrhoids
Small and asymptomatic external hemorrhoids don’t require any treatment, although most patients experience intermittent flare-ups. Surgery (external hemorrhoidectomy) may be needed in the case of large external hemorrhoids and/or persistent, symptomatic external hemorrhoids.
What is Rubber Band Ligation?
Rubber band ligation (RBL) is a common treatment method for hemorrhoids, especially prolapsed hemorrhoids, in Minnesota. This office procedure is almost never appropriate for grade 1 or mild grade 2 hemorrhoids (which are treated with IRC) or more severe grade 4 hemorrhoids (which are treated with surgery). RBL involves a doctor inserting a scope into the anus and clamping onto the prolapsed hemorrhoid to place a rubber band around its base, cutting off the blood flow to the hemorrhoid and causing it to shrink and die off. The procedure only takes a few minutes but is usually limited to one hemorrhoid per office visit. RBL downgrades hemorrhoids to grades 1 or 2, and any remaining hemorrhoids are typically treated with infrared coaguation (IRC).
After RBL, most patients can return to regular activities (except heavy lifting) almost immediately. Some patients may feel tightness, mild pain, or an urge for bowel movements; a few patients may also experience slight rectal bleeding. If significant rectal bleeding occurs, call your doctor immediately. Tylenol/Ibuprofen and sitz baths can help relieve pain and discomfort post-surgery.
Does Pregnancy Cause Hemorrhoids?
Hemorrhoids are very common during pregnancy, affecting 20-50 percent of pregnant women. While some women experience pre-existing hemorrhoids, others often develop them during first-time pregnancy and may have recurring hemorrhoids later on due to the following:
Symptoms include anal itching, rectal bleeding, pain, and bulging out. Hemorrhoids typically worsen in the third trimester, after labor, and in conjuction with constipation. However, symptoms usually improve significantly following childbirth with the help of home remedies like ointments, fiber supplements, sitz baths and cold packs. If painful external hemorrhoids develop, then a simple surgery using incision and drainage is necessary to remove blood clots and alleviate rectal pain. For severe cases, a limited external hemorrhoidectomy may be required. Patients are encouraged to undergo a hemorrhoid evaluation 2-3 months after delivery if they experienced severe or recurring hemorrhoids during pregnancy.
When Should I Call a Doctor From the Hemorrhoid Clinic?
While home remedies can temporarily relieve hemorrhoid symptoms, they fail to address the root cause of the hemorrhoids and, thus, aren’t practical long-term treatment methods. It’s best to speak with a doctor for an accurate diagnosis and treatment plan that will permanently rid you of hemorrhoids, while also checking for signs of colon or rectal cancer.
See a doctor ASAP if you experience any of the following symptoms: rectal bleeding, black stool, an anal lump, abdominal symptoms (bloating, diarrhea or constipation), thin, small-sized stool, worsening of current hemorrhoids, and changing or worsening rectal symptoms.
What Are Common Causes of Rectal Lumps?
A rectal lump is a growth in the anal canal or rectal area that can vary in size and severity. Depending on its underlying cause, a rectal lump may or may not be painful. Causes can include anal warts, hemorrhoids, polyps, fissures, or cancer.
Hemorrhoids are the most common cause of rectal lumps. The lump can be a prolapsed internal hemorrhoid or an external hemorrhoid, with thrombosed external hemorrhoids (varicose veins rupture and blood clots develop) being the most painful and severe.
Anal warts are caused by the human papilloma virus (HPV). An HPV infection is considered a sexually transmitted disease and, if left untreated, can spread and increase the risk of cancer in the anorectal region.
An anal fissure is a small cut or split in the anal lining often caused by a painful, hard bowel movement. Fissures are typically found anterior or posterior to the anus and is often associated with a lump called sentinel pile, accompanied by pain and bleeding.
Anal polyps are growths in the anal canal that must be removed and examined further to check for proximal lesions in the rectum and colon.
Anal cancer occurs in the anal canal and accounts for two percent of cancer in the gastrointestinal tract. An external or internal mass may be palpable. Anal or rectal cancer generally does not produce any pain; the cancer can take several forms including ulcers, polyps or verrucous growths.
What is the Easy Hemorrhoid Care™ (EHC) Program?
The Easy Hemorrhoid Care™ (EHC) Program is a new care delivery system for treating hemorrhoids using minimally invasive procedures, including Infrared Coagulation (IRC), rubber band ligation, and modified hemorrhoidectomy. It is a low-stress, efficient system that requires only one office trip and successfully reduces discomfort, risk of complications, and recovery time. This comfortable and seamless experience provides enhanced, customized hemorrhoid care, saving you precious time in your busy schedule.
Standard hemorrhoid care typically consists of multiple office visits using Infrared Coagulation and/or rubber banding ligation for internal hemorrhoid treatments, followed by an external hemorrhoidectomy and/or excision of anal hemorrhoids. It’s a long process, but it’s usually covered by your medical insurance. Easy Hemorrhoid Care™ (EHC), while NOT covered by insurance, is far more efficient, advanced, and ideal for a safer and easier recovery.
To learn more about our Easy Hemorrhoid Care™ experience at One Stop Medical Center, please call us at 952-922-2151, or email us at info@shuMD.com.
What Are Common Causes of Anal Itching?
There are two types of anal itching: primary (no definitive cause) and secondary (itching acts as symptom of an underlying medical issue). Potential causes include:
What Should I Know About Anal Cancer?
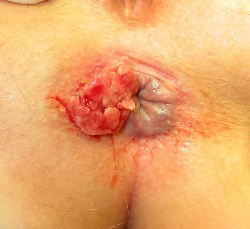 Anal cancer accounts for two percent of cancers that occur in the gastrointestinal tract and usually refers to anal squamous cell carcinoma, a disease associated with human papillomavirus (HPV). Anal cancer develops when the squamous cells in the anal canal become inflamed.
Anal cancer accounts for two percent of cancers that occur in the gastrointestinal tract and usually refers to anal squamous cell carcinoma, a disease associated with human papillomavirus (HPV). Anal cancer develops when the squamous cells in the anal canal become inflamed.
Symptoms – Usually no painful symptoms, although an external or internal mass may be palpable. Anal/pelvic pain, anal bleeding, sensation of a mass in the rectum, local sensations of wetness/irritation, prolapse, rectal incontinence, and severe constipation may also occur. Patients with anal cancer often mistake their rectal symptoms for hemorrhoids, which then leads to a delayed diagnosis.
Risk Factors – Active HPV infection, smoking, receiving anal sex, immunosuppression, HIV infection, and organ transplant
Prevention – Vaccination against HPV serotypes 16 and 18, which are believed to cause the majority of cases, is the best way to prevent the development of anal cancer.
Treatment – Surgery used in limited capacity (usually for early stages of anal cancer). Most patients undergo radiation therapy with radiosensitizing chemotherapeutic agents, which may produce short-term adverse effects of chemotherapy and long-term risks of radiation exposure. Conservative management of symptoms include lifestyle changes and bulking agents and anti-diarrheal agents.
How Do You Differentiate Anal Fissures From Hemorrhoids?
Although hemorrhoids and anal fissures are both related to rectal pain and rectal bleeding, they are two very different conditions. Hemorrhoids are usually only mildly painful and aren’t always related to bowel movements. Anal fissures, however, produce sharp rectal pain during bowel movements.
An anal fissure is a tear in the anal canal in the lower rectum. They’re usually caused by trauma from a hard or painful bowel movement and lack of dietary fiber. Symptoms include severe rectal pain during bowel movements, which worsens with constipation. Slight rectal bleeding may also occur.
About 80 percent of fissures resolve themselves without surgery. Initial treatment involves fiber supplements, stool softeners and laxatives to aid in improving bowel movements. Sitz baths are also encouraged. If these initial steps don’t work, 0.4% nitroglycerine (NTG) ointment or Nifedipine gel may be recommended. For more severe cases, botox can help relax the anal sphincters long enough for the fissure to heal. A partial anal sphincterotomy can also be performed, where a cut is made on the sphincter so that both the fissure and new cut can heal together.
Why Are Infected Hemorrhoids So Rare?
The rarity of hemorrhoid infections has to do with the body’s unique immune system response to small tears. When a small tear or hemorrhoid occurs, an immediate inflammatory/clotting response around the broken blood vessels prevents bacteria from spreading deeper into the surrounding tissue. Any bacteria that DOES make it past the initial barrier are targeted via non-inflammatory antibodies known as “IgA,” which is why there are no symptoms typically associated with infection (swelling, pain, itching, etc).
However, this immune system response typically only applies to smaller tears. A large tear or injury increases the risk of infection, so it’s important to seek treatment for more severe hemorrhoid cases.
What is the Correct Way to Use Hemorrhoid Cream?
Over-the-counter (OTC) hemorrhoid cream is a widely available and effective treatment option to temporarily improve symptoms of irritation, itching and swelling. However, it doesn’t actually fix the underlying cause of the hemorrhoid, so it’s crucial to still see a doctor for a full examination and treatment plan.
Many patients fail to correctly use hemorrhoid cream. Whether the cream is applied externally or internally depends on each patient’s symptoms. If you experience symptoms toward the outside of the anus, apply the cream externally:
• Using your finger, apply a small amount around the outside of your anus
• Use the cream 2-3 times daily
• Wash your hands after each application
• Use the cream no more than a week each course. Stop application once symptoms improve or disappear.
• Continue using the cream if symptoms recur
If external use doesn’t work, or if you know that you have internal swelling, apply the cream internally:
• Try to have a bowel movement prior to using the cream
• Fill the applicator with the tube of cream
• Lubricate the end of the applicator with petroleum jelly
• Gently insert the applicator into your rectum
• Squeeze the tube of cream gently
• Remove and wash the applicator, as well as your hands
• Try not to have a bowel movement within two hours after an application
• Use the cream no more than a week each course. Stop application once symptoms improve or disappear
• Continue using the cream if symptoms recur
What’s the Difference Between Hemorrhoids and Anal Abscesses?
Although both hemorrhoids and anal abscesses appear to be tissue lumps protruding from the rectum, they are two very different conditions. Anal abscesses are an infection around the opening of the anus or deep in the rectum, where there is pus. They are commonly mistaken for hemorrhoids but are more painful and can lead to fever. Anal abscess is an acute disease rather than a chronic condition, and it’s important to seek medical attention if symptoms are found.
Anorectal abscesses are the result of infection of anal glands in the lining of the anal canal near the opening of the anus. When bacteria from the gut passes the anal sphincter barrier and into the surrounding tissue of the rectum, an abscess of varying severity and depth forms. Anal abscesses most commonly occur in men, as well as patients who are in their 30s and 40s. Most abscess can be identified through a physical exam and digital rectal examination, although deep abscesses may require a CT scan, MRI scan, or ultrasonography to confirm.
Treatment – Surgical incision and drainage should be performed ASAP, as antibiotics are ineffective at this stage of the infection. Delaying surgery can result in tissue destruction, fibrosis (scar tissue formation), and impaired anal continence. Drainage involves making a small incision above the abscess as close to the anus as possible, then removing the gauze after 24 hours. Sitz baths and stool softeners can help with post-surgery discomfort.
What Are Common Causes of Minor Rectal Bleeding?
Minor rectal bleeding occurs when small amounts of bright, red, fresh blood from the rectum/anus appear on stool, toilet paper, or in the toilet bowl. Any amount of rectal bleeding should be taken very seriously.
Common causes include internal hemorrhoids, ruptured thrombosed external hemorrhoids, fissures, fistulas, diverticulosis, colon cancer, colitis, and polyps. The source of the bleeding is determined by patient history, a physical exam and endoscopies. Initial inspection for anal warts, anal fissures, cancer or external hemorrhoids is performed, followed by a digital examination and anoscopy to detect any abnormalities and sources of bleeding in the lower rectum and anal canal. A sigmoidoscopy or colonoscopy may also be done. The management of minor rectal bleeding mainly focuses on treating underlying diseases.
Patients who should be further examined include: older patients, those with significant family history of bowel disease or cancer, and those previously treated for rectal bleeding but continue to experience bleeding.
How Do You Treat External Thrombosed Hemorrhoids?
Thrombosed external hemorrhoids occur when varicose veins rupture and blood clots develop, leading to swelling and severe pain.
Less severe cases can be treated with non-surgical methods like stool softeners, increased fiber and fluid intake, Sitz baths and analgesia. Most patients, however, require surgical excision, a safe and effective office procedure performed under local anesthesia. During this simple procedure, the hemorrhoid is cut open, and the blood clots are removed, preventing risk of recurrence. An external hemorrhoidectomy may also be performed, where the hemorrhoidal tissue with blood clots is removed together, and the bleeding in the wound is stopped with a cautery. The wound in the anal area is covered with sterile gauze.
Following surgery, patients should take warm Sitz baths three times daily, keep hydrated, and take stool softeners.
What is Proctalgia Fugax (Fleeting Rectal Pain)?
Proctalgia fugax (fugax meaning “fleeting” in Latin) is a condition that causes severe episodic pain in the anorectal area due to spasms in the levator ani, the main pelvic floor muscle. Episodes, which can last a few seconds to 30 minutes, typically occur at night and are often mistaken as an urge to defecate. While it doesn’t physically harm the body, proctalgia fugax can be painful and debilitating.
This condition typically starts around the age of 45. Roughly 8-18 percent of people have it, but only 20-30 percent of those affected seek medical help. While proctalgia fugax cannot be cured, its symptoms can be managed using the following methods:
What is the Recovery Process for an External Hemorrhoidectomy?
Most external hemorrhoidectomies are performed under local anesthesia, so patients are able to go home immediately afterward. For patients who undergo general anesthesia, they must remain in the office until the sedative wears off.
Once home, patients should take a couple days off work and avoid any intense physical straining. However, remaining active to help blood circulation is still important! Any soreness and discomfort in the bowel region can be managed with Tylenol or Ibuprofen; stronger painkillers, while discouraged, are an option for more severe post-operative pain. Sitz baths should be taken three times daily, 15-20 minutes per session. This helps the wound heal better and prevents chance of infection. The anus should also be kept clean and dry. To help ease bowel movements, use stool softeners and increase fiber and fluid intake.
Full recovery should take about 2-3 weeks.
How Do You Find a Qualified Hemorrhoid Doctor?
Hemorrhoid procedures are usually conducted by colorectal surgeons, general surgeons and family physicians. Below are some tips on finding a qualified doctor who can provide complete hemorrhoid care.
1. Check the doctor’s credentials. Experience matters!
- How many hemorrhoid procedures does the doctor perform each week?
- How many years of hemorrhoid care does he/she have?
- Does he/she provide complete hemorrhoid care by offering all treatment options, including IRC, banding and surgeries?
- What is his/her complication rate?
- Does the doctor offer a convenient and alternative hemorrhoid care delivery system?
2. Ask if the doctor uses newer, non-surgical technologies or surgical techniques. Because not every patient needs a hemorrhoidectomy, it’s important to know what each doctor offers in terms of both non-surgical and surgical care. Some family doctors only offer hemorrhoid creams, while other surgeons only offer a hemorrhoidectomy. Treatment plans should be customized based on each patient’s needs.
3. Use local sources for research. These include Google searches, insurance companies and primary care doctors. Feedback from family and friends who have undergone hemorrhoid treatment can provide invaluable, in-depth information on finding a good doctor.
4. Once you have a few options, narrow down your search. While credentials and clinical experience are extremely important, there are also practical considerations that can indicate the extent to which each doctor is committed to hemorrhoid care:
Review the doctor’s website to see if:
Ask about the total cost.
Look for a hemorrhoid care system that is friendly and patient-oriented. For example, One Stop Medical Center offers Easy Hemorrhoid Care with a one-trip care system.
Consider the office location and commute convenience.
Evaluate the quality of customer service. Pay attention to how a patient is treated on the phone, the cleanliness of the office, the staff’s attitudes, the quality of the procedure room, etc.
What Are the Best & Worst Foods to Eat When You Have Hemorrhoids?
Knowing the right kinds of food to incorporate into your daily diet can make a major difference in treating and preventing hemorrhoid flare-ups. Shoot for 25-50 grams of fiber everyday. Too much fiber in one sitting can cause gas and bloating, so be sure to add it to your diet in small increments. Below is a quick and dirty breakdown of the best and worst foods to consume while dealing with hemorrhoids:
BEST FOODS
EAT plenty of fruits and vegetables – Apples, berries, broccoli, leafy greens and winter squash are great options!
EAT whole grains – Oatmeal is one of the most popular whole grain foods, as well as whole grain breads, brown rice and popcorn.
EAT more legumes (beans, lentils, nuts) – Black beans, almonds, chickpeas and edamame contain large amounts of fiber even in very small portions.
EAT flax, hemp and chia seeds – These are all good sources of soluble fiber.
DRINK LOTS OF WATER – Aim for at least eight cups of water daily.
WORST FOODS
AVOID refined grains– White bread, bagels, white rice and pretty much anything made from white flour.
AVOID processed foods – Fast food, frozen meals and pre-packaged junk food contain few nutrients, tons of sodium, and inflammation-promoting ingredients.
AVOID excessive alcohol – Alcohol dehydrates your body and can lead to constipation and disrupt the digestive balance in your stomach.
AVOID dairy – Milk and cheese products often cause gas and bloating, which can contribute to hemorrhoid pain and stomach cramps if you are already constipated.
AVOID fried, salty food – Fries, fried chicken, fritters, the list goes on. These items are not only difficult to digest, but also cause your body to hang onto water, putting more pressure on your blood vessels.
AVOID spicy food – Again, inflammation.
What Are Everyday Habits That Contribute to Hemorrhoid Development?
While major lifestyle changes, such as pregnancy, can cause hemorrhoid development, many cases actually develop from seemingly insignificant everyday habits that build up over time. Below are a few common habits to be mindful of if you’re worried about hemorrhoids:
Not enough fiber – Low fiber intake can lead to constipation, which causes overstraining during bowel movements and inflamed veins. Aim for 25-50 grams of fiber everyday.
Straining/overexerting during workouts – Suddenly increasing weight amounts too quickly puts a burst of pressure on your lower region.
Sitting too long on the toilet – Hemorrhoids usually worsen when there’s an increased, downward pressure, so avoid adding pressure to the veins.
Eating too much processed food – Fast food, frozen meals and pre-packaged junk food contain few nutrients, tons of sodium, and inflammation-promoting ingredients.
Sitting for long periods of time – Decreased mobility can cause blood flow to also decrease, and blood is more likely to gather up/pool in the anal veins, causing irritation and swelling.
Not hydrating enough – Drinking more fluids promotes good digestion and proper stool passage. Aim for at least eight cups of water daily.
If you do develop hemorrhoids, you may be able to alleviate discomfort using these home remedies. However, it’s important to still visit your doctor for a full examination and treatment rundown.
What Kind of Exercises Help Alleviate Hemorrhoid Symptoms?
One important activity that can significantly assist your hemorrhoid prevention progress is exercising, which can include anything from simple walking to more intense cardio workouts.
Kegel Exercises – This strengthen the muscles in the pelvic area and increases blood flow to the anal region. Strong anal muscles provide good support for internal hemorrhoids while also preventing existing ones from enlarging or protruding. Similar to squeezing your pelvic region when you feel the need to urinate, squeeze and hold that same movement for five seconds. Release and relax for five seconds. Repeat this exercise 10 times per session, three times daily.
Brisk Walking – The goal is to improve blood flow to your pelvic region, so walking 20-30 minutes regularly keeps your body upright rather than sedentary on a couch. Begin by walking slowly to warm up. Increase your pace after a few minutes to increase your heart rate and improve your body’s blood circulation.
Aerobics/Cardio Workouts – Aerobic exercises (running, swimming, spinning/cycling, dancing, aerobics classes) get the blood flowing and help relax any strained muscles in the lower part of the body. Performing aerobics—or other forms of cardio—improves blood circulation to the pelvic/anal regions, while also helping with constipation, one of the primary causes of hemorrhoids.



