Hemorrhoids Online Registration
Hemorrhoids are swollen, bulging blood vessels in the walls of the anus and lower rectum. When the tissues supporting the vessels become inflamed and stretch, the vessels expand and cause its walls to thin. This often leads to bleeding. If the intense stretching and internal pressure continue, these already weakened vessels ultimately protrude from the anus.
Prevalence and Risk Factors
The exact prevalence of hemorrhoids is unknown, but it’s estimated that roughly half of Americans develop hemorrhoids by age 50. Approximately 10 million people in the US are affected, with one million new cases reported each year.
While hemorrhoids can develop at any age, most cases occur in patients over 30, with a peak in those between 45-60 years old. External hemorrhoids tend to be more common in younger adults. Although men seem to be more likely to seek medical attention, pregnancy can increase the chance of symptomatic hemorrhoids, as well as thrombosis, in women.
There are no indicative factors to identify which individuals are more predisposed to hemorrhoids. Caucasians are affected by—and seek treatment for—symptoms more often than other races. Those who 1) live in rural areas and 2) have higher socioeconomic status seem to be more prone to developing hemorrhoids.
Types of Hemorrhoids
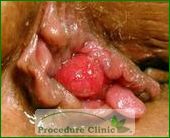 Patients with hemorrhoids can suffer from internal hemorrhoids, external hemorrhoids, or mixed hemorrhoids. Internal hemorrhoids develop inside the rectum and form above the dentate line, while external hemorrhoids form below the dentate line. Mixed hemorrhoids refer to the presence of both internal and external hemorrhoids.
Patients with hemorrhoids can suffer from internal hemorrhoids, external hemorrhoids, or mixed hemorrhoids. Internal hemorrhoids develop inside the rectum and form above the dentate line, while external hemorrhoids form below the dentate line. Mixed hemorrhoids refer to the presence of both internal and external hemorrhoids.
External hemorrhoids form below the dentate line and are visible outside the opening of the rectum. These cases are especially irritating during and after bowel movements, which can cause further anal itching and swelling. Thrombosed external hemorrhoids are more severe cases that occur when varicose veins in the anal skin rupture and cause blood clots, which leads to swelling and a bluish-purple discoloration. External hemorrhoids are typically treated with either incision and removal of the clot or with an external hemorrhoidectomy, as simple drainage of the clot can lead to recurrence.
Internal hemorrhoids, found inside the rectum, are graded from I to IV based on the hemorrhoid’s degree of prolapse. Grade I hemorrhoids have no prolapse. Grade II lesions bulge with defecation but then recede spontaneously. Grade III hemorrhoids require digital replacement after prolapsing, while grade IV hemorrhoids cannot be reduced once prolapsed.
The Four Cardinal Symptoms of Hemorrhoids
Although hemorrhoidal symptoms and complaints are common and typically not a serious concern, all patients should be examined for signs of possible cancer and other associated diseases. There are four primary symptoms for hemorrhoids—anal itching, anal pain, rectal lumps and rectal bleeding.
Anal Itching – This symptom comes and goes, but worsens when hemorrhoids flare up. Because the itching happens sporadically, many patients incorrectly assume that the temporary relief means the problem resolved itself. Continuous scratching or excessive cleaning of the anal area may further harm the sensitive tissues and worsen symptoms.
Anal Pain – Because internal hemorrhoids form inside the anus, they’re usually not painful. However, patients may experience mild aching and discomfort during flare-ups. This pain can escalate if complications develop, such as thrombosis, infection and sphincter spasms (Proctalgia Fugax). In the case of external thrombosed hemorrhoids, immediate onsets of intense pain may occur and last anywhere from a few days to a couple of weeks.
Rectal Lumps – A palpable anal lump typically accompanies external hemorrhoids; thrombosed external hemorrhoids often cause very painful, bluish lumps due to the hemorrhoidal veins rupturing and causing blood clots. In the case of internal hemorrhoids, a rectal lump typically becomes larger and more prolapsed immediately following a bowel movement. A lump can also be associated with other symptoms such as bleeding, itching or pain.
Rectal Bleeding – While this is the most common symptom of hemorrhoids, the severity of rectal bleeding varies widely from case to case. Besides hemorrhoids, conditions such as ruptured thrombosed external hemorrhoids, fissures, diverticulosis, colon cancer, colitis, polyps and angiodysplasias can also cause rectal bleeding. Any amount of rectal bleeding should be addressed ASAP.
Hemorrhoid Treatments
Click here for more details on treatment options based on hemorrhoid type and severity. Because no single treatment modality can fix all hemorrhoids, a hemorrhoid clinic will offer multiple treatment modalities to meet a patient’s specific needs and provide complete care.
Hemorrhoid Prevention
 Because hemorrhoids is a varicose vein disease, recurrence is possible even after treatment, especially in advanced hemorrhoid cases. While this can be extremely frustrating for patients, there are numerous measures available to help prevent hemorrhoid relapse.
Because hemorrhoids is a varicose vein disease, recurrence is possible even after treatment, especially in advanced hemorrhoid cases. While this can be extremely frustrating for patients, there are numerous measures available to help prevent hemorrhoid relapse.
Dietary changes – Eat more fiber! Low fiber intake often leads to constipation and overstraining during bowel movements. This pressure then strains your varicose veins and significantly increases your risk of developing hemorrhoids. Make a point to eat a diet rich in fruits, vegetables and whole grain.
Improved bowel habits – As mentioned above, constipation and poor bowel habits can rupture your hemorrhoidal veins, so it’s ideal to keep your stool soft. This can be achieved with a high-fiber diet, increased water intake, bulking agents and stool softeners, all of which can help prevent overstraining. It’s also best to avoid sitting on the toilet for too long, as residual feces can irritate the anal skin. You can consider programming your bowel movements according to your shower schedule so that the anal area is cleaned afterward.
Weight loss – Obese patients in Minnesota are 2-4 times more likely to develop hemorrhoids than the average patient, so being mindful of overall diet and weight is recommended.
Treating underlying conditions – Individuals with other medical conditions, such as liver cirrhosis with portal hypertension, cardiovascular diseases, and abdominal tumors are more likely to develop hemorrhoids. Treating these underlying diseases is an important part of preventing future hemorrhoids.
If you do experience a hemorrhoid relapse, you should immediately request treatment from an experienced practitioner in Minnesota. One Stop Medical Center serves the entire Twin Cities and offers comprehensive hemorrhoid treatment plans.



