Anal Itching
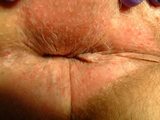
Treatments for anal itching include taking antihistamine as a sedative prior to sleeping to prevent the patient from unconsciously scratching, or using a topical corticosteroid to alleviate the itching. Underlying disorders such as hemorrhoids must be considered and treated when diagnosing and treating anal itching.
Anal pain
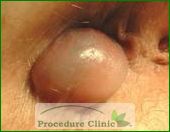 Anal pain is a common sign of anorectal disease. Pain caused by an acute anal fissure may occur during intense, forced bowel movements that are often accompanied by rectal bleeding. Pain that begins gradually and becomes excruciating may indicate infection, and occurrence of fever and inability to urinate indicates need for emergency treatment. Immediate onsets of intense pain accompanied by a palpable mass are usually a result of an external thrombosed hemorrhoid, which may last a few days to a couple of weeks. Internal hemorrhoids, however, are not painful due to being located above the dentate line of the rectum. Similarly, rectal cancer typically does not cause pain unless the condition is advanced. The patients with chronic anal fissures usually have intermittent sharp rectal pain and bleeding with each bowel movement for a long time.
Anal pain is a common sign of anorectal disease. Pain caused by an acute anal fissure may occur during intense, forced bowel movements that are often accompanied by rectal bleeding. Pain that begins gradually and becomes excruciating may indicate infection, and occurrence of fever and inability to urinate indicates need for emergency treatment. Immediate onsets of intense pain accompanied by a palpable mass are usually a result of an external thrombosed hemorrhoid, which may last a few days to a couple of weeks. Internal hemorrhoids, however, are not painful due to being located above the dentate line of the rectum. Similarly, rectal cancer typically does not cause pain unless the condition is advanced. The patients with chronic anal fissures usually have intermittent sharp rectal pain and bleeding with each bowel movement for a long time.
Proctalgia fugax is a more serious anal pain condition that involves short spasms of intense pain at night. This condition may occur once each year or up to three or four times each week. The pain is typically accompanied by sweating and an urge to pass stool. There is currently no treatment for proctalgia fugax, but placing oneself in hot water or applying ice may provide symptomatic relief.
Rectal Lump
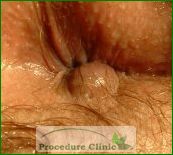
- Hemorrhoids are probably the most common reason for having a rectal lump. It can be caused by internal hemorrhoids, but more commonly by external hemorrhoids. If a rectal lump is related to internal hemorrhoids, it usually gets bigger and more prolapsed right after the bowel movement; it could be spontaneously reduced in the early stage of internal hemorrhoids. But it could be non-reducible in the late stage of hemorrhoids. It may be associated with other symptoms such as bleeding, itch or pain. The thrombosed external hemorrhoids are usually very painful if the varicose veins rupture and the blood clots develop.
- Anal warts are caused by human papilloma virus (HPV). HPV infection is considered to be sexually transmitted diseases. Left untreated, anal warts can spread and increase the risk of cancer in the rectal and anal region.
- Anal Fissure is a small cut or split in the anal lining often caused by a painful, hard bowel movement. Fissures are typically located anterior or posterior to the anus. Anal fissure is often associated with a lump called sentinel pile, accompanied by pain and bleeding.
- Anal cancer occurs in the anal canal, it is account for 2% of cancer in the gastrointestinal tract. An external or internal mass may be palpable. Anal or rectal cancer generally do not produce any pain; Some lesions are so soft that they are missed on palpation. Anal cancer can take several forms including ulcers, polyps or verrucous growths.
Rectal bleeding
Rectal bleeding refers to the passage of red blood from the rectum and anus, often mixed with stool and/or blood clots. The severity of rectal bleeding varies widely. Most rectal bleeding is mild and intermittent, but it also may be moderate or severe.
Rectal bleeding can be caused by various conditions, but even the slightest amount of bleeding should be taken seriously. Common causes of bleeding are internal hemorrhoids, ruptured thrombosed external hemorrhoids, fissures, diverticulosis, colon cancer, colitis, polyps and angiodysplasias. Patients of older age or with significant family history of bowel disease or cancer should consider further examination. In addition, patients who were previously treated for rectal bleeding but continued to experience bleeding must be further examined.
The source of rectal bleeding is determined by history, physical examination and blood tests, assisted with anoscopy, sigmoidoscopy, colonoscopy, radionuclide scans, and angiograms.



