Hemorrhoids Online Registration
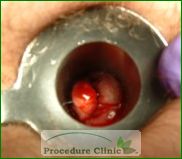
How is rubber band ligation (RBL) performed?
The process involves a doctor inserting an anoscope into the anus and grasping the prolapsed hemorrhoid to place a rubber band around its base. With the rubber band in place, the hemorrhoid shrinks and recedes, dying off in a few days or a week. The reduced volume of venous tissue with the scar formation prevents hemorrhoid tissue from bulging into the anal canal. The procedure is done in a doctor’s office and takes only a couple of minutes. Treatment is limited to 1-2 hemorrhoids per office visit; additional areas may be treated in two-week intervals.
What should I expect after rubber band ligation (RBL) treatment?
After the procedure, you shouldn’t feel much discomfort, although some patients may feel tightness, mild pain, or an urge to have a bowel movement. While different patients respond differently to this procedure, most are able to return to regular activities almost immediately; others may need a few hours or a day of rest.
If you experience any pain after banding, you may use Tylenol or Ibuprofen as needed and take plenty of warm sitz baths for 15-30 minutes at a time to relieve discomfort. Some patients may have slight rectal bleeding in a week when the hemorrhoid dies off. This bleeding usually stops by itself; however, if you notice significant rectal bleeding, please call your doctor’s office. It is also very important to make sure that your stool is soft by taking stool softeners containing fiber and drinking more fluids to help prevent hemorrhoids in the future.



