The most common presentation of hemorrhoid disease is rectal bleeding, pain, itcing, or prolapse. Because these symptoms are extremely nonspecific and may be seen in a number of anorectal diseases, the physician must therefore perform an adequate rectal examinationto (including anoscopy) to confirm the diagnosis.
Minor rectal bleeding is one of the common symptoms that the hemorrhoid patients seek for the medical care. Most hemorrhoidal bleeding occurs with bowel movement, and it is caused by passing stool, particularly hard stools, and a lot of times that bleeding is a bright red in nature, and it may drip into the toilet sometimes.
 Severe pain is not a common symptom of hemorrhoids, because internal hemorrhoid happens in the area above the dentate line that is supplied by the visceral nerve, like those found within the intestines, which sense pressure rather than pain. Mild aching pain and skin iritating pain in the rectum is common because of local inflammation.
Severe pain is not a common symptom of hemorrhoids, because internal hemorrhoid happens in the area above the dentate line that is supplied by the visceral nerve, like those found within the intestines, which sense pressure rather than pain. Mild aching pain and skin iritating pain in the rectum is common because of local inflammation.
As the vessel complex of an internal hemorrhoid becomes varicose and continues to enlarge, it bulges into the anal canal and loses its normal anchoring, becoming a prolapsing internal hemorrhoid. The prolapsing hemorrhoid usually returns into the anal canal or rectum on its own after bowel movement, or can be pushed back inside using one’s finger, but usually prolapses again after the next bowel movement.
The rectal mucosal lining that has been pulled down secretes mucus and moistens the anus and its surrounding skin, while the stool itself can also leak onto the anal skin. Itchiness often occurs as a result of this dual presence of stool and moisture.
In general, symptoms of external hemorrhoids are different than those of internal hemorrhoids. External hemorrhoids can be felt as bulges at the anus, but rarely display any of the same symptoms seen with internal hemorrhoids. Occasionally, the external hemorrhoids or anal tag turns out to be quite large, which can make anal hygiene (cleaning) difficult or irritate the anus.
When the varicose vein complex of hemorrhoids ruptures, blood clots occur and build up the pressure inside the lump. This condition, known as thrombosed external hemorrhoid, causes an extremely painful bluish anal lump and often requires medical attention. The somatic nerve in the anal canal (below the dentate line) can sense pain, this is why the patients feel significant pain when they develop thrombosed external hemorrhoids. Thrombosed hemorrhoids may heal with scarring and leave a tag of skin protruding from the anus.
 We used to believe that hemorrhoidal bleeding is venous. Now the evidence indicates that hemorrhoidal bleeding is arterial, which is supported by the bright red color and arterial pH of the blood.
We used to believe that hemorrhoidal bleeding is venous. Now the evidence indicates that hemorrhoidal bleeding is arterial, which is supported by the bright red color and arterial pH of the blood.  When you think of medical conditions or illnesses related to Minnesotans, you may assume something along the lines of frostbite, pneumonia, dry skin, or just anything related to the state’s extremely cold winters. However, a study of the most frequently Googled health condition in every US state in the past year revealed that the Land of 10,000 Lakes is most concerned about…
When you think of medical conditions or illnesses related to Minnesotans, you may assume something along the lines of frostbite, pneumonia, dry skin, or just anything related to the state’s extremely cold winters. However, a study of the most frequently Googled health condition in every US state in the past year revealed that the Land of 10,000 Lakes is most concerned about…
 While Botox is often associated with battling wrinkles and fine lines on the face, the medication can actually be used in your…anal region. But not for cosmetic purposes, of course.
While Botox is often associated with battling wrinkles and fine lines on the face, the medication can actually be used in your…anal region. But not for cosmetic purposes, of course. Constipation is one of the most common bowel disorders affecting American adults, with roughly 20 percent of the population suffering from hard, painful stools. Defined as having fewer than three bowel movements per week for several weeks, constipation occurs when the colon absorbs too much water from the food passing through it, creating dry stool that’s extremely difficult to pass.
Constipation is one of the most common bowel disorders affecting American adults, with roughly 20 percent of the population suffering from hard, painful stools. Defined as having fewer than three bowel movements per week for several weeks, constipation occurs when the colon absorbs too much water from the food passing through it, creating dry stool that’s extremely difficult to pass. 3. Exercise more – Being more active is always beneficial to your health! Hitting the gym or simply going for a jog outside helps aid food breakdown and reduce the time it takes food to move through the large intestine. The less time food sits in your colon, the more water it retains to help ease stool passage later.
3. Exercise more – Being more active is always beneficial to your health! Hitting the gym or simply going for a jog outside helps aid food breakdown and reduce the time it takes food to move through the large intestine. The less time food sits in your colon, the more water it retains to help ease stool passage later. Although the exact causes of skin tags are unclear, they usually result from one or more of the following:
Although the exact causes of skin tags are unclear, they usually result from one or more of the following: The average American spends over five hours per day scrolling through Instagram feeds, checking Twitter, answering emails and texts, and watching Netflix—all via smartphone devices and, more often than not, while sitting. Add in the extra layer of using these mobile devices during bathroom trips, and most of us have significantly increased our risk of developing hemorrhoids.
The average American spends over five hours per day scrolling through Instagram feeds, checking Twitter, answering emails and texts, and watching Netflix—all via smartphone devices and, more often than not, while sitting. Add in the extra layer of using these mobile devices during bathroom trips, and most of us have significantly increased our risk of developing hemorrhoids. Your doctor will then insert a light-equipped device called an anoscope into your lower gastrointestinal tract via the anus. An anoscope is a small, hollow, rigid tube roughly 3-5 inches long and 2 inches wide and is usually coated with a jelly-like substance to help ease insertion. While the device is being inserted, your doctor may also ask you to clamp and relax your internal muscles to help with the placement of the anoscope.
Your doctor will then insert a light-equipped device called an anoscope into your lower gastrointestinal tract via the anus. An anoscope is a small, hollow, rigid tube roughly 3-5 inches long and 2 inches wide and is usually coated with a jelly-like substance to help ease insertion. While the device is being inserted, your doctor may also ask you to clamp and relax your internal muscles to help with the placement of the anoscope. Yes, you read that correctly—elephant foot yam is loaded with potential medicinal benefits and may even improve hemorrhoidal symptoms. This alternative medicine has long been used in Ayurveda, a traditional system of medicine rooted in the Indian subcontinent whose practices have recently been globalized. Used to treat numerous conditions such as sperm quality, liver and spleen disorders, and hemorrhages, elephant foot yam just may be the next big home remedy for treating hemorrhoids as well.
Yes, you read that correctly—elephant foot yam is loaded with potential medicinal benefits and may even improve hemorrhoidal symptoms. This alternative medicine has long been used in Ayurveda, a traditional system of medicine rooted in the Indian subcontinent whose practices have recently been globalized. Used to treat numerous conditions such as sperm quality, liver and spleen disorders, and hemorrhages, elephant foot yam just may be the next big home remedy for treating hemorrhoids as well. When considering
When considering 
 If you’ve ever experienced an itchy bum in the middle of the night, it’s quite an unpleasant sensation. Scratching the area may provide temporary relief, but the harshness of your nails ends up causing further irritation and damage to the already sensitive anal region.
If you’ve ever experienced an itchy bum in the middle of the night, it’s quite an unpleasant sensation. Scratching the area may provide temporary relief, but the harshness of your nails ends up causing further irritation and damage to the already sensitive anal region. While the term
While the term  Hemorrhoids, abscesses, fistulas, fissures, anal itching, rectal prolapse—with so many anorectal disorders out there, it’s hard to keep track of which is which. Two of these conditions, anal abscesses and anal fistulas, are closely linked to one another but can be easily distinguished via the guidelines below.
Hemorrhoids, abscesses, fistulas, fissures, anal itching, rectal prolapse—with so many anorectal disorders out there, it’s hard to keep track of which is which. Two of these conditions, anal abscesses and anal fistulas, are closely linked to one another but can be easily distinguished via the guidelines below. Bleeding from your rectum or anus is never a pleasant experience, and it can understandably cause immediate panic. Generally, bright red blood indicates bleeding in the lower rectum, while dark red blood indicates bleeding from deeper and further up in the body. While passing dark red blood is usually a sign of digestive bleeding and requires immediate attention,
Bleeding from your rectum or anus is never a pleasant experience, and it can understandably cause immediate panic. Generally, bright red blood indicates bleeding in the lower rectum, while dark red blood indicates bleeding from deeper and further up in the body. While passing dark red blood is usually a sign of digestive bleeding and requires immediate attention,  After rubber band ligation, you’ll typically experience a bit of pain and a feeling of fullness in the lower abdomen, as well as an urge to have a bowel movement. These sensations are totally normal and usually subside within a few days. You may also experience small amounts of anal/rectal bleeding for about 7 days after procedure due to the hemorrhoid falling off. It’s encouraged to avoid physically intense activities that strain the body for at least 2-3 weeks. While some patients are able to return to regular activities immediately, others may need a couple days of downtime and bed rest.
After rubber band ligation, you’ll typically experience a bit of pain and a feeling of fullness in the lower abdomen, as well as an urge to have a bowel movement. These sensations are totally normal and usually subside within a few days. You may also experience small amounts of anal/rectal bleeding for about 7 days after procedure due to the hemorrhoid falling off. It’s encouraged to avoid physically intense activities that strain the body for at least 2-3 weeks. While some patients are able to return to regular activities immediately, others may need a couple days of downtime and bed rest. Hemorrhoids have plagued humans for thousands of years, with the earliest known mention of its symptoms dating back to roughly ~2250 BC in the kingdom of Babylon in the Code of King Hammurabi. Fast forward to 1700 BC in Egypt, and we stumble upon the first-ever recorded case of hemorrhoids, which also happened to highlight an important topical wound ointment.
Hemorrhoids have plagued humans for thousands of years, with the earliest known mention of its symptoms dating back to roughly ~2250 BC in the kingdom of Babylon in the Code of King Hammurabi. Fast forward to 1700 BC in Egypt, and we stumble upon the first-ever recorded case of hemorrhoids, which also happened to highlight an important topical wound ointment. Dealing with hemorrhoid discomfort can be a real pain (literally). In addition to visiting your doctor for a full exam,
Dealing with hemorrhoid discomfort can be a real pain (literally). In addition to visiting your doctor for a full exam,  2. Straining/overexerting yourself during workouts – If a weight is too heavy, DON’T force yourself. Suddenly increasing weight amounts too quickly puts a burst of pressure on your lower region, which is NOT what you want for your blood vessels.
2. Straining/overexerting yourself during workouts – If a weight is too heavy, DON’T force yourself. Suddenly increasing weight amounts too quickly puts a burst of pressure on your lower region, which is NOT what you want for your blood vessels. 5. Sitting for long periods of time – It’s not just excessive toilet-sitting that’s frowned upon. Sitting and binge-watching four straight hours of Keeping Up With the Kardashians will essentially produce the same negative results. Decreased mobility can cause blood flow to also decrease, and blood is more likely to gather up/pool in the anal veins, causing irritation and swelling that can develop into hemorrhoids.
5. Sitting for long periods of time – It’s not just excessive toilet-sitting that’s frowned upon. Sitting and binge-watching four straight hours of Keeping Up With the Kardashians will essentially produce the same negative results. Decreased mobility can cause blood flow to also decrease, and blood is more likely to gather up/pool in the anal veins, causing irritation and swelling that can develop into hemorrhoids.

 Because the symptoms of hemorrhoids and early-stage rectal/colon cancer are very similar, people often confuse and, at times, misdiagnose the two conditions. Since the treatment method for each condition is vastly different, it’s important to know how to differentiate hemorrhoids from rectal cancer and proceed with the appropriate treatment options.
Because the symptoms of hemorrhoids and early-stage rectal/colon cancer are very similar, people often confuse and, at times, misdiagnose the two conditions. Since the treatment method for each condition is vastly different, it’s important to know how to differentiate hemorrhoids from rectal cancer and proceed with the appropriate treatment options.


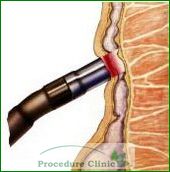
 IRC offers major advantages to patients over previous hemorrhoid treatment methods:
IRC offers major advantages to patients over previous hemorrhoid treatment methods: Anoscopy is a simple medical procedure that can help your doctor identify an abnormality in your anus and distal rectum.
Anoscopy is a simple medical procedure that can help your doctor identify an abnormality in your anus and distal rectum.


