No longer will you have to fear hemorrhoid treatment — Infrared coagulation (IRC) of hemorrhoids is a fast and effective non-surgical solution.
A hemorrhoid is a common illness that numerous Minnesotans suffer from. It is estimated that more than 10 million people in the United States suffer from hemorrhoids. Approximately three out of four people will develop hemorrhoids at some time in their lives. Dr. Steven Shu, an office proceduralist, commonly treats hemorrhoids and can quickly alleviate your pain.
While many people associate hemorrhoids with painful surgery, only a small percentage of patients actually require surgery. A fast and simple office procedure has taken the fear out of hemorrhoid treatment. The majority of hemorrhoids patients are good candidates for non-surgical treatment, or Infrared coagulation (IRC).
What is Infrared Coagulation (IRC) of Hemorrhoids?
Infrared Coagulation (IRC) is a safe, fast, and effective solution for hemorrhoids. It is approved by the FDA for the treatment of hemorrhoids. This office-based procedure takes just a few minutes and uses infrared light to treat symptomatic internal hemorrhoids. Therefore, IRC has quickly become the most widely used office procedure for hemorrhoids and is preferred over other methods because it is fast, effective, well-tolerated by patients, and rarely has complications.
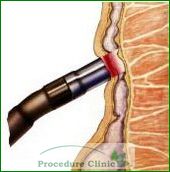
A small light probe contacts the area above the hemorrhoid complex under direct view, exposing the tissue to a burst of infrared light for about one second. This coagulates the veins above the hemorrhoid, causing it to shrink.
Since the hemorrhoids are located in an area that is full of sensitive somatic nerve endings (same as the nerves in skin), it is too painful to coagulate the hemorrhoids directly because they are too close to the opening of the anus. Fortunately, many small veins that feed the hemorrhoids lie in an area that is supplied with sympathetic nerve endings, which is not as sensitive as the somatic nerves in skin.
With IRC, your doctor can effectively coagulate the insensitive area right above the hemorrhoids and destroy these small veins. In this way, the sensitive and painful area is avoided, and IRC becomes a very tolerable treatment.
By destroying these small veins with IRC, it stops the flow of blood to the varicose veins of hemorrhoids, just like blocking many small rivers will dry up a large lake.
IRC offers major advantages to patients over previous hemorrhoid treatment methods:
• Fast, simple, and safe solution
• No anesthesia required
• No special preparation needed
• No recovery time after treatment
• Clinically proven results
• Covered by all major insurance companies
Who are the Best Candidates for Infrared Coagulation (IRC)?
Infrared coagulation can be used to treat the early stages of hemorrhoids, and it is most effective in grade 1-2 hemorrhoids. If you’re suffering from irritating internal hemorrhoids that continue to cause itching, discomfort, pain, bleeding and other symptoms, and it does not respond to conservative self-management, IRC treatments might be a good solution.
How is Infrared Coagulation Procedure Performed?
Before IRC procedure is performed, Dr. Shu gently inserts the anoscope (a very short, 3-4 inch rigid metal tube), then uses a handheld device that creates an intense beam of infrared light to touch the mucosa above the hemorrhoids, exposing the hemorrhoid tissue to a quick pulse of infrared light. The heat from the infrared light burns 4-5 spots in the targeted area, coagulating the vein above the hemorrhoids.
The resulting scar tissue cuts off the blood supply to the hemorrhoid venous complex. This causes the hemorrhoid complex to shrink and die. It may take a few weeks for all the hemorrhoids to shrink completely. Moreover, the scar tissue acts to hold nearby hemorrhoid veins in place so they don’t bulge into the anal canal easily and become hemorrhoids as you age.
Each IRC treatment only takes a couple of minutes. You may need as many as four separate treatment sessions every two weeks to cover all the areas where hemorrhoids appear, but this depends on each individual case and how extensive your hemorrhoids are.
What is the Recovery Time of Infrared Coagulation Procedure?
After the IRC procedure, you may feel mild discomfort in the anus and the urge to have a bowel movement sometimes. You are able to resume normal everyday activities immediately afterward. Typically, there are no post-treatment effects. However, there may be slight spot bleeding a few days later, but heavy rectal bleeding is extremely rare. Avoid heavy straining, lifting, and aspirin. If you notice significant rectal bleeding, you should call your doctor’s office.
You may use Tylenol as needed and take a warm sitz bath daily to relieve discomfort. A stool softener, fiber, and water will help ease your bowel movement while you heal.
Dr. Shu has had extensive experience in treating hemorrhoids with non-surgical IRC treatments in the past two decades, and he has successfully treated about two thousand hemorrhoids patients with almost ten thousand IRC treatments. Please call 952-922-2151 if you need help to treat your symptomatic hemorrhoids.
 Hemorrhoids are swollen blood vessels in the rectal and anal area. They can occur internally or externally and are typically caused by increased pressure in the lower rectum. Factors contributing to this pressure include straining during bowel movements, chronic constipation or diarrhea, obesity, pregnancy, and even genetic predisposition. Hemorrhoids can be uncomfortable, causing symptoms like pain, itching, bleeding, and discomfort during bowel movements.
Hemorrhoids are swollen blood vessels in the rectal and anal area. They can occur internally or externally and are typically caused by increased pressure in the lower rectum. Factors contributing to this pressure include straining during bowel movements, chronic constipation or diarrhea, obesity, pregnancy, and even genetic predisposition. Hemorrhoids can be uncomfortable, causing symptoms like pain, itching, bleeding, and discomfort during bowel movements. Hemorrhoids are swollen blood vessels in the rectum or anus that can cause pain, itching, bleeding, and discomfort during bowel movements. They can be internal (inside the rectum) or external (outside the anus). Lifestyle factors, constipation, pregnancy, and genetics are common contributors to their development.
Hemorrhoids are swollen blood vessels in the rectum or anus that can cause pain, itching, bleeding, and discomfort during bowel movements. They can be internal (inside the rectum) or external (outside the anus). Lifestyle factors, constipation, pregnancy, and genetics are common contributors to their development.
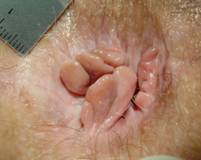 Have you been using too much toilet paper because of pesky anal tags? Hemorrhoidal skin tags (piles) are flaps of skin or flesh found around the anus. They often form as a result of an existing hemorrhoids.
Have you been using too much toilet paper because of pesky anal tags? Hemorrhoidal skin tags (piles) are flaps of skin or flesh found around the anus. They often form as a result of an existing hemorrhoids.  As the venous complex of an internal hemorrhoid becomes varicose and continues to enlarge, it bulges into the anal canal and loses its normal anchoring, becoming a prolapsing internal hemorrhoid. The prolapsing hemorrhoid usually returns into the anal canal or rectum on its own, or can be pushed back inside using one’s finger, but usually prolapses again after the next bowel movement. In the anal canal, a hemorrhoid is exposed to movement caused by passing stool, particularly hard stools that can cause bleeding and sting pain. The painless rectal bleeding with bright red blood is a common symptom of internal hemorrhoids. The rectal mucosal lining that has been pulled down secretes mucus and moistens the anus and its surrounding skin, while the stool itself can also leak onto the anal skin. Itchiness often occurs as a result of this dual presence of stool and moisture.
As the venous complex of an internal hemorrhoid becomes varicose and continues to enlarge, it bulges into the anal canal and loses its normal anchoring, becoming a prolapsing internal hemorrhoid. The prolapsing hemorrhoid usually returns into the anal canal or rectum on its own, or can be pushed back inside using one’s finger, but usually prolapses again after the next bowel movement. In the anal canal, a hemorrhoid is exposed to movement caused by passing stool, particularly hard stools that can cause bleeding and sting pain. The painless rectal bleeding with bright red blood is a common symptom of internal hemorrhoids. The rectal mucosal lining that has been pulled down secretes mucus and moistens the anus and its surrounding skin, while the stool itself can also leak onto the anal skin. Itchiness often occurs as a result of this dual presence of stool and moisture.













 When you think of medical conditions or illnesses related to Minnesotans, you may assume something along the lines of frostbite, pneumonia, dry skin, or just anything related to the state’s extremely cold winters. However, a study of the most frequently Googled health condition in every US state in the past year revealed that the Land of 10,000 Lakes is most concerned about…
When you think of medical conditions or illnesses related to Minnesotans, you may assume something along the lines of frostbite, pneumonia, dry skin, or just anything related to the state’s extremely cold winters. However, a study of the most frequently Googled health condition in every US state in the past year revealed that the Land of 10,000 Lakes is most concerned about…
 Your doctor will then insert a light-equipped device called an anoscope into your lower gastrointestinal tract via the anus. An anoscope is a small, hollow, rigid tube roughly 3-5 inches long and 2 inches wide and is usually coated with a jelly-like substance to help ease insertion. While the device is being inserted, your doctor may also ask you to clamp and relax your internal muscles to help with the placement of the anoscope.
Your doctor will then insert a light-equipped device called an anoscope into your lower gastrointestinal tract via the anus. An anoscope is a small, hollow, rigid tube roughly 3-5 inches long and 2 inches wide and is usually coated with a jelly-like substance to help ease insertion. While the device is being inserted, your doctor may also ask you to clamp and relax your internal muscles to help with the placement of the anoscope. When considering
When considering 
 If you’ve ever experienced an itchy bum in the middle of the night, it’s quite an unpleasant sensation. Scratching the area may provide temporary relief, but the harshness of your nails ends up causing further irritation and damage to the already sensitive anal region.
If you’ve ever experienced an itchy bum in the middle of the night, it’s quite an unpleasant sensation. Scratching the area may provide temporary relief, but the harshness of your nails ends up causing further irritation and damage to the already sensitive anal region. While the term
While the term  After rubber band ligation, you’ll typically experience a bit of pain and a feeling of fullness in the lower abdomen, as well as an urge to have a bowel movement. These sensations are totally normal and usually subside within a few days. You may also experience small amounts of anal/rectal bleeding for about 7 days after procedure due to the hemorrhoid falling off. It’s encouraged to avoid physically intense activities that strain the body for at least 2-3 weeks. While some patients are able to return to regular activities immediately, others may need a couple days of downtime and bed rest.
After rubber band ligation, you’ll typically experience a bit of pain and a feeling of fullness in the lower abdomen, as well as an urge to have a bowel movement. These sensations are totally normal and usually subside within a few days. You may also experience small amounts of anal/rectal bleeding for about 7 days after procedure due to the hemorrhoid falling off. It’s encouraged to avoid physically intense activities that strain the body for at least 2-3 weeks. While some patients are able to return to regular activities immediately, others may need a couple days of downtime and bed rest. Dealing with hemorrhoid discomfort can be a real pain (literally). In addition to visiting your doctor for a full exam,
Dealing with hemorrhoid discomfort can be a real pain (literally). In addition to visiting your doctor for a full exam,  2. Straining/overexerting yourself during workouts – If a weight is too heavy, DON’T force yourself. Suddenly increasing weight amounts too quickly puts a burst of pressure on your lower region, which is NOT what you want for your blood vessels.
2. Straining/overexerting yourself during workouts – If a weight is too heavy, DON’T force yourself. Suddenly increasing weight amounts too quickly puts a burst of pressure on your lower region, which is NOT what you want for your blood vessels. 5. Sitting for long periods of time – It’s not just excessive toilet-sitting that’s frowned upon. Sitting and binge-watching four straight hours of Keeping Up With the Kardashians will essentially produce the same negative results. Decreased mobility can cause blood flow to also decrease, and blood is more likely to gather up/pool in the anal veins, causing irritation and swelling that can develop into hemorrhoids.
5. Sitting for long periods of time – It’s not just excessive toilet-sitting that’s frowned upon. Sitting and binge-watching four straight hours of Keeping Up With the Kardashians will essentially produce the same negative results. Decreased mobility can cause blood flow to also decrease, and blood is more likely to gather up/pool in the anal veins, causing irritation and swelling that can develop into hemorrhoids.

 Because the symptoms of hemorrhoids and early-stage rectal/colon cancer are very similar, people often confuse and, at times, misdiagnose the two conditions. Since the treatment method for each condition is vastly different, it’s important to know how to differentiate hemorrhoids from rectal cancer and proceed with the appropriate treatment options.
Because the symptoms of hemorrhoids and early-stage rectal/colon cancer are very similar, people often confuse and, at times, misdiagnose the two conditions. Since the treatment method for each condition is vastly different, it’s important to know how to differentiate hemorrhoids from rectal cancer and proceed with the appropriate treatment options.




 Anoscopy is a simple medical procedure that can help your doctor identify an abnormality in your anus and distal rectum.
Anoscopy is a simple medical procedure that can help your doctor identify an abnormality in your anus and distal rectum.